Source: United States Breastfeeding Committee
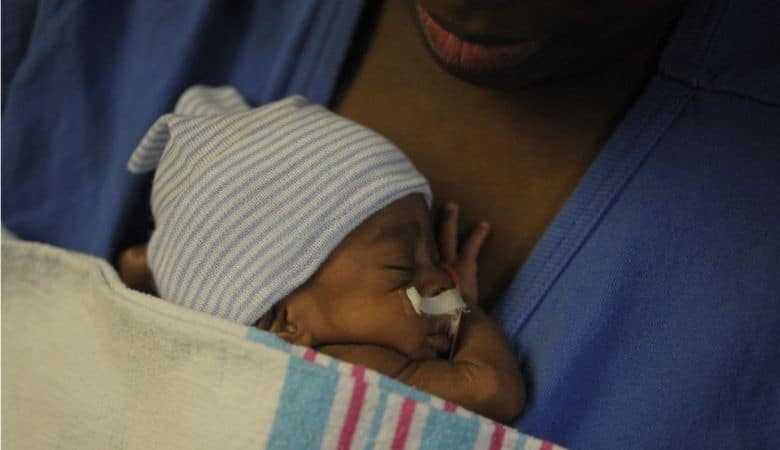
November is Prematurity Awareness Month.
While there is much overlap, prematurity and NICU are not synonymous. Some NICU babies are full term with birth-related or congenital diseases requiring special care. Prematurity does not end when babies go home from the NICU.
Fetal growth occurs over 39-40 weeks of pregnancy. When babies are born early, this growth is incomplete. Development is very different when you have to breathe, eat, fight germs, and keep warm on your own than when those services are part of the in utero package. It takes time to catch up. Preterm babies have two birth dates—the chronological date and the adjusted or corrected age. Specialists use adjusted age for 2 -2 ½ years after birth, and some effects of prematurity are lifelong.
Long-term outcomes of prematurity
Thanks to advances in care over the last few decades, many babies born as early as 22-23 weeks and under 1 pound can now survive and thrive. They are reaching adulthood in greater numbers than ever before, giving providers and researchers the opportunity to learn about long-term outcomes of extreme prematurity. This is helping improve care for today’s preterm babies in the NICU and as they grow.
Extremely preterm babies are more likely to experience asthma, cerebral palsy, hypertension, mood and anxiety disorders, attention deficit disorder, developmental delays, and epilepsy. These are generally identified and treatments begun by the time the children reach school age. Some are outgrown, many are lifelong. A recent study indicates that over ¾ of babies born before 27 weeks have at least one chronic health condition when they reach adolescence or young adulthood—considerably more than their full-term cohort.
Risk factors for chronic disease, including high blood pressure and pulmonary (lung) and cardiac (heart) problems, often do not become apparent until adulthood. While it is not yet fully understood, babies born very early, who must finish growing their hearts, lungs, brains, and eyes while they are using them, often have long-term risks.
Preterm birth as a chronic condition
As more babies are born earlier and living to become healthy and productive adults, “preterm birth should be thought of as a chronic condition that requires long-term follow-up . . . Doctors are not used to seeing them, but they increasingly will,” observed Dr. Casey Crump, family physician and epidemiologist. This requires education, training, and research well beyond neonatology and pediatrics.
Several areas of ongoing research are improving prognoses for extremely preterm babies:
- NICU care involves balancing medications to support lung, heart, eye, and brain growth, prevent and treat infections such as necrotizing enterocolitis (NEC) and sepsis, and ensure that the medications complement one another—all in a 1- or 2-pound baby.
- We understand the importance of human milk (mom’s own and donor milk) for growth, brain development, and infection prevention. Still, these babies should be receiving their nourishment from the umbilical cord and infection protection from the amniotic sac for the next several months. Nutrition for extremely preterm babies is a crucial and active area of research and practice.
- There is also promising research on social interventions. For example, a recent study in Rhode Island placed babies and their families in private NICU rooms and followed up at home with regular check-ins and a 24/7 helpline. These interventions resulted in 30% higher milk production; higher scores on cognitive and language tests at age 2; lower health care costs; and fewer hospital visits, a significant problem for preterm babies.
Expanding the prematurity awareness tent
Thanks to scientific and medical advances, it’s time to expand the prematurity awareness tent to include the adults who were premature babies and their ongoing health care providers. Welcome to the tent. There is much to celebrate and to learn.
Naomi Bar-Yam, PhD, ACSW, is available to speak at hospitals, community organizations, and conferences on prematurity, the role of families on the NICU team, milk banking, and many other topics. Visit her speaker profile on LactSpeak.